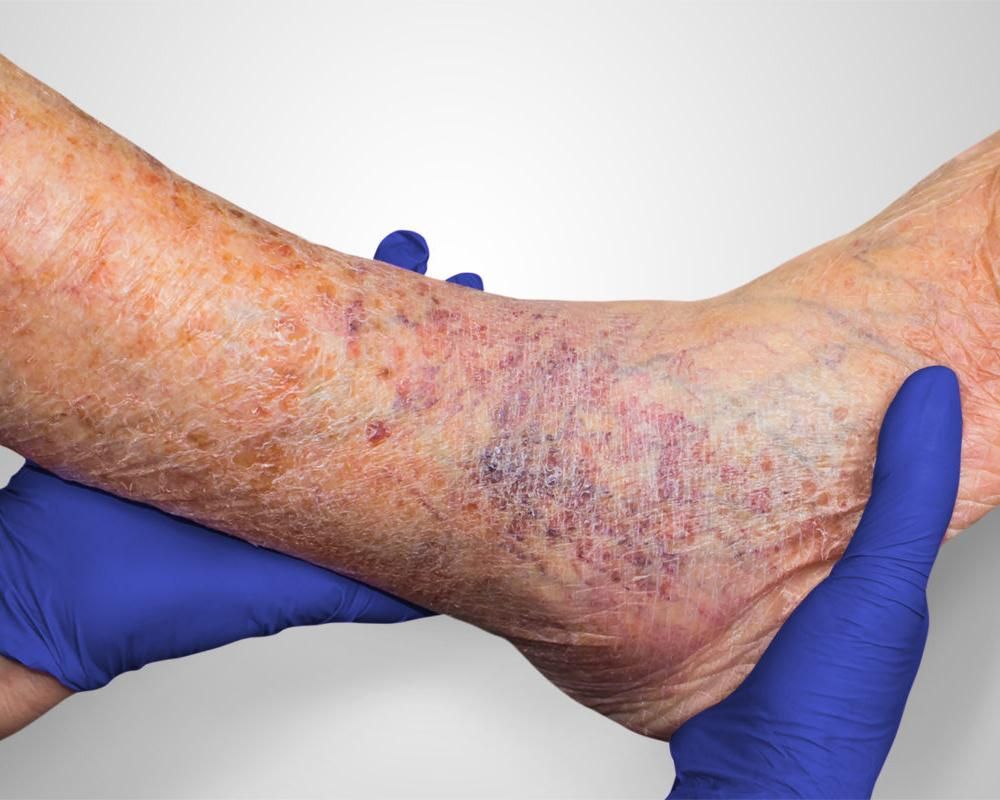
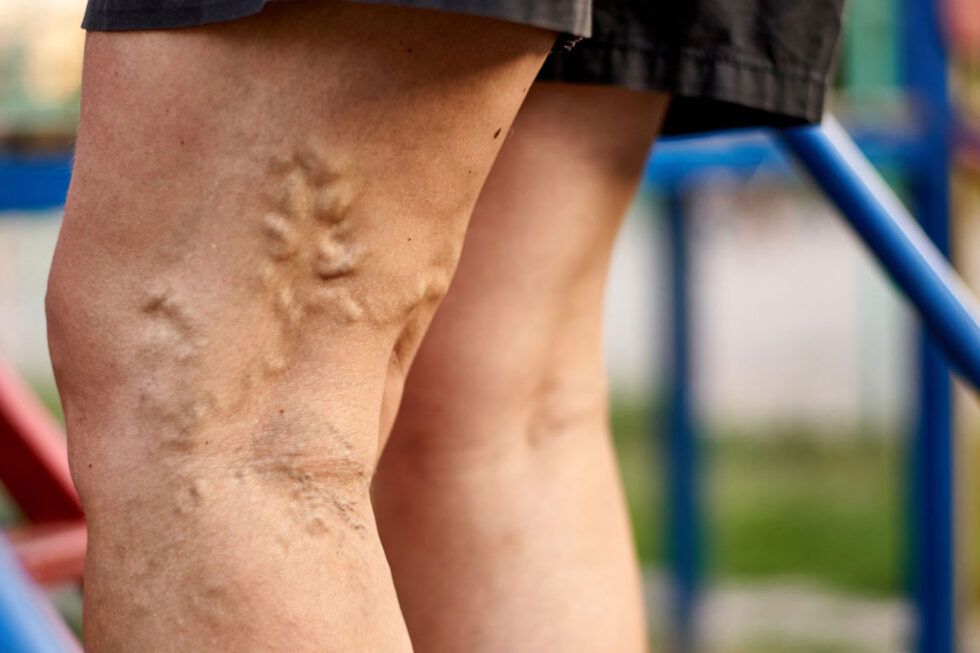
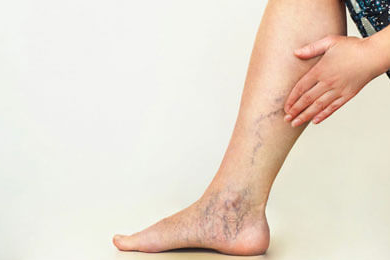
Leg Swelling and Lymphedema
Leg swelling is not a rare complaint and may occur for many reasons. It happens due to the accumulation of body fluids in the lower extremities. If both legs are swollen, it indicates some generalized disease condition, like heart disease, kidney issues, and even medication side effects. In some, even prolonged periods of immobility may lead to leg swelling.
Since leg swelling may occur due to many causes like heart disease, venous insufficiency, infection, injury, or lymphatic failure, a thorough investigation is the only way to find the actual cause.
However, leg swelling from lymphedema differs. Quite often, doctors may even confirm its diagnosis through physical examination. Nevertheless, doctors would need to carry out specific tests to confirm the diagnosis.
What is lymphedema?
Quite like the circulatory system, a small amount of fluid circulates in the body throughout the lymphatic system. It primarily helps fight against infections, carry out toxins and wastes, and help transport lymphocytes throughout the body. The lymph is also rich in proteins.
In certain situations, obstruction of the lymph flow may occur, leading to the build-up of lymph in some tissues. This build-up of the lymph is called lymphedema. Although it may affect various parts of the body, lymphedema of the lower legs is the most common.
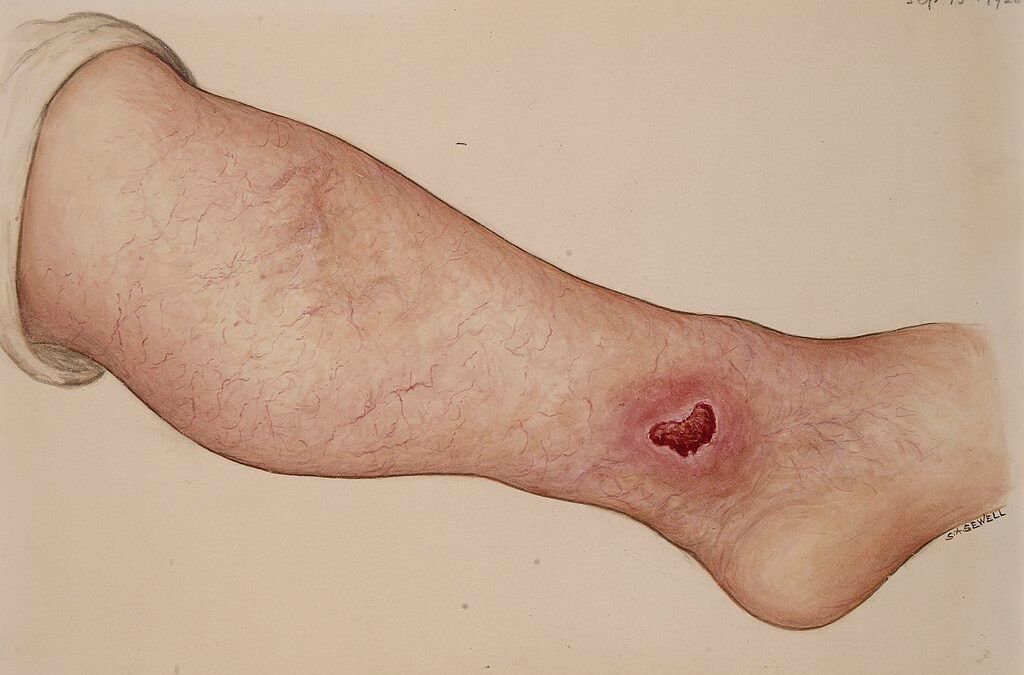
Generally, lymphedema starts with swelling that is noticeable at the end of the day. However, it may subside after prolonged rest, like during the night. Nonetheless, if the condition progresses, it may cause a permanent build-up of lymph in the legs.
Causes of lymphedema
It is a common practice to divide the causes of lymphedema into two groups; primary and secondary.
Lymphedema is primary when it occurs due to some congenital disease or failure of development of the lymphatic system after birth. However, the definition of primary lymphedema is a bit controversial, as it may also include lymphedema of unknown cause. Nevertheless, some examples of primary lymphedema are congenital, Milroy disease, lymphedema tarda, and so on.
Secondary lymphedema occurs due to obstruction or disruption of the lymphatic system. It may occur due to cancer, cancer treatment, trauma, surgery, infection, and even parasitic infection like filariasis. Among these reasons, filariasis, a parasite that blocks the lymph flow and thus causes severe lymphedema is endemic only in sub-tropical parts of the world like South Asia, South America, the Caribbean, and parts of Africa.
In the US and other developed nations, perhaps the leading cause of lymphedema is the surgical removal of lymph nodes, mostly done during cancer treatment. It is estimated that as many as 7-77% of patients may develop lymphedema after axillary lymph node dissection (ALND). However, it may also occur due to scarring caused by radiotherapy.
Phlebolymphedema as one of the most overlooked causes of lymphedema
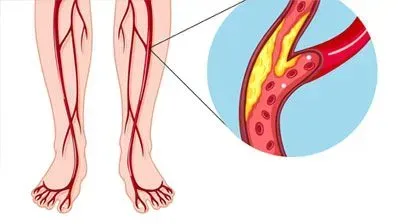
Apart from the above causes, it appears that in the US and Western world, perhaps the most common cause of lymphedema is due to venous insufficiency. This is a type of secondary lymphedema. It often has a mixed cause: venous hypertension leads to poor lymph flow and resulting lymphedema or leg swelling. Due to its mixed nature, it is quite challenging to manage as there is both an overloading of the venous and lymphatic systems.
How will doctors diagnose lymphedema?
In most cases, doctors would be able to differentiate lymphedema from other causes of swelling based on the patient’s clinical history and with the help of a physical examination. Nevertheless, it is worth understanding that effective early diagnosis of the conditions is vital as it may affect the success of the treatment in many cases. In addition, studies show that about one-third of all such swellings are transient.
However, it may require further investigation if the swelling is more persistent. Additionally, some investigations may also help understand the severity of the condition.
Doctors would commonly use various imaging methods to understand the condition better. Thus, some of the widely used imaging methods are lymphoscintigraphy, MRI, CT scan, and ultrasonography. Ultrasonography is often preferred due to its ease of use and safety profile, as it does not involve exposing patients to radiation.
However, doctors may also use other non-imaging methods to understand lymph flow, like bioimpedance spectroscopy and tonometry.
Doctors may also do staging of the severity of the condition. In stage 0, there are no swellings of extremities, and visible signs of lymphedema are absent. The diagnosis of stage 0 is mainly based on the results of imaging studies like lymphoscintigraphy.
In stage 1, there is already visible lymphedema. However, it is relieved with prolonged rest or elevating the limbs. In stage 2, the elevation of lower limbs does not relieve the edema. Stage 2 is also the beginning of the hardening of the limbs due to fibrosis. In stage 3,the tissue becomes fibrotic and hard, and they also become irresponsive to pressure application; thus, debulking surgery is the only option in this stage.
Treatment options for lymphedema
Lymphedema is mostly treated without pharmacological drugs. Thus, exercise may help improve the lymph flow in mild cases, especially when combined with adequate rest.
Some massage therapists may also help improve lymph flow with the help of manual therapy. It may also help prevent blood clots and help enhance the quality of the skin.
Compression bandages may be quite helpful in many cases. For example, one may use compression bandages to wrap the entire limb so that lymph can readily flow back. Compression garments could also be another excellent option. Additionally, specialists may use a technique called lymph taping to improve drainage from areas that are difficult to wrap in bandages.
For more severe cases, there are some devices like sequential pneumatic compression. It contains a sleeve that is worn over the affected area and then pumps intermittently inflates and deflates the sleeve, thus boosting the lymph flow.
Finally, there are also surgical options of treatment for more severe cases. All surgical methods can be broadly divided into two groups. One approach is to improve lymph flow through bypass surgery. The second way is a debulking therapy used to remove fibrous tissues. Again, surgical methods are generally reserved for more severe cases when non-invasive methods fail to help.
However, again, treatment choice would greatly depend on the cause and stage of lymphedema. For example, treating venous issues will also be necessary in the case of mixed lymphedema caused by insufficiency of both the venous and lymphatic systems. In addition, venous issues may require additional treatment methods like the use of venous stenting to improve venous back flow.
References
- Murdaca G, Cagnati P, Gulli R, et al. Current Views on Diagnostic Approach and Treatment of Lymphedema. The American Journal of Medicine. 2012;125(2):134-140. doi:10.1016/j.amjmed.2011.06.032
- Kayıran O, De La Cruz C, Tane K, Soran A. Lymphedema: From diagnosis to treatment. Turk J Surg. 2017;33(2):51-57. doi:10.5152/turkjsurg.2017.3870
- Farrow W. Phlebolymphedema–A Common Underdiagnosed and Undertreated Problem in the Wound Care Clinic. J Am Col Certif Wound Spec. 2010;2(1):14-23. doi:10.1016/j.jcws.2010.04.004
- Greene AK, Goss JA. Diagnosis and Staging of Lymphedema. Semin Plast Surg. 2018;32(1):12-16. doi:10.1055/s-0038-1635117
- Schaverien MV, Coroneos CJ. Surgical Treatment of Lymphedema. Plastic and Reconstructive Surgery. 2019;144(3):738-758. doi:10.1097/PRS.0000000000005993
- Raju S, Furrh JB, Neglén P. Diagnosis and treatment of venous lymphedema. Journal of Vascular Surgery. 2012;55(1):141-149. doi:10.1016/j.jvs.2011.07.078